Phlebitis
What is Phlebitis and what are the symptoms?
The word phlebitis is made up of two parts:
- “Phleb” – meaning “vein”
- “itis” – which is usually put on the end of a medical word to mean “inflammation”
Thus “phlebitis” simply means inflammation in the veins. However, veins virtually never become inflamed without any reason at all. The commonest cause of phlebitis that occurs naturally is when a clot forms in a vein near the surface and the vein becomes inflamed, which is the natural reaction of a vein to a clot within it and the way clots are removed naturally.
Phlebitis of the legs
We will now return to the most common type of phlebitis – phlebitis that is associated with varicose veins or hidden varicose veins (caused by venous incompetence or venous reflux disease).
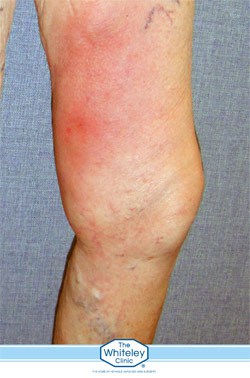
Firstly, we need to understand why the clot occurs in varicose veins or hidden varicose veins. In normal leg veins, blood flows up the veins when pumped by the foot or leg muscles on exercise. When the leg is not exercising, the blood starts to fall down the leg and is stopped by valves. In people with varicose veins or hidden varicose veins (caused by venous incompetence or venous reflux disease) these valves have stopped working.
In this case, blood is still pumped up the veins normally on movement. However, when the leg relaxes, the valves are not functioning and so blood falls down the leg veins due to gravity. The valves are said to be “incompetent” and the blood is “refluxing” back down the leg veins in the opposite direction to normal.
This abnormal backward flow of blood increases the amount of blood in the leg veins and, once this reflux has been going on for several years, some of the vein walls weaken and start dilating. If these dilated veins are seen on the surface, they are called “varicose veins”. However, if they are too deep to be seen on the surface, they will not be visible. But they are there and dilated and so act just like any visible varicose veins.
Historically there has been no name given to these veins. We now call them “hidden varicose veins” for obvious reasons and, whenever we talk about hidden varicose veins, we know they are caused by venous incompetence (the valves not working) and venous reflux disease (the blood falling the wrong way down the veins with gravity).
In the 1800’s a German doctor called Rudolf Virchow (1821-1902) identified the causes of what makes blood clot within a vein. There are three causes and these are called “Virchow’s Triad”. Virchow’s triad shows that blood will clot if any one of the following occurs:
- 1 – there is a change in the vessel wall
- 2 – there is a change in the flow of blood within the vessel
- 3 – there is a change in the blood constituents
In varicose veins and hidden varicose veins, both the vessel wall has changed due to dilatation and also flow has changed as the blood is now refluxing rather than being stopped by normal valves. As such, in certain circumstances, blood can clot within these varicose veins or hidden varicose veins.
When blood clots within a vein, it is called a “thrombosis”. When a thrombosis occurs within a vein, it irritates the wall, setting into action a chain of events resulting in inflammation of the vein wall and surrounding tissue. This inflammation is nature’s way of trying to heal the clot or thrombosis. Inflammation increases the local blood supply and brings white blood cells to the area, which will eat away the clot over time.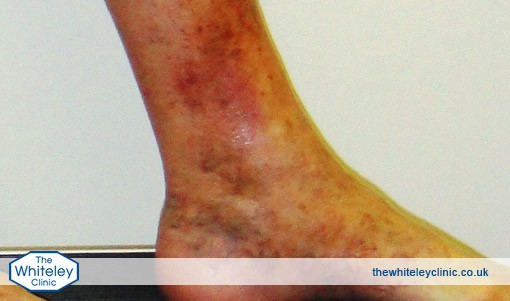
However in some patients, before this can happen, the clot can extend which can cause major problems. If the clot extends into the deep veins, it can become a deep vein thrombosis (DVT). In addition, if that clot flies off in the venous blood flow, it can go through the heart and into the lungs a very serious condition called pulmonary embolism (PE). Until recently, it was thought that phlebitis could not cause any major medical problems and so treatment was quite simple – aspirin and compression stockings. However recent studies have shown that it is essential to get an urgent duplex ultrasound scan and on the results of this, anticoagulation treatment may be needed to stop deep-vein thrombosis (DVT) and pulmonary embolism (PE).
It is very important to note at this point that the inflammation is due to thrombosis (clot) within the vein and NOT any infection. As we will see later, doctors and nurses who do not understand phlebitis will often prescribe antibiotics purely and simply because the vein is hot, tender and red. These are the signs of inflammation, which, in phlebitis, is due to healing and NOT infection. Therefore antibiotics will have absolutely no effect on phlebitis.
Facts about Phlebitis
Phlebitis is commonly misdiagnosed and more importantly it is very often mistreated.
Essential facts about phlebitis:
- Phlebitis is due to blood clots in the superficial veins
- Antibiotics are NOT a treatment for Phlebitis
- Everyone with Phlebitis must have a duplex ultrasound scan
- Treatment is dictated by scan results:
- Anticoagulation (ie: warfarin) if the clot is within 5cm of the deep veins
- Asprin and support stockings if the clot is more than 5cm from deep veins
- Phlebitis can cause a clot to the lung if not treated correctly
It has now been shown, by studies in America and the UK, that Phlebitis in the veins in the legs can give rise to clots that travel to the lungs. These clots are called Pulmonary Emboli (PE’s) and they can be life threatening.
Most patients with Phlebitis are not at risk of PE’s. However without a duplex scan, it is impossible to tell which patients with Phlebitis are at risk and which patients are not.
The symptoms and signs of phlebitis
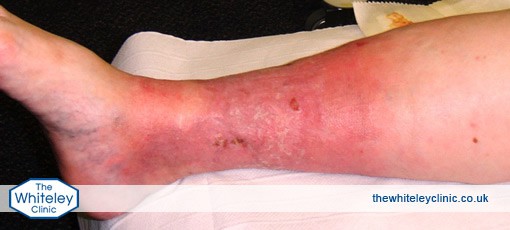
Hot, red, lumpy veins in the legs – are due to blood clots in the veins just under the surface. These clots cause the vein and surrounding tissues to become inflamed. There is no infection so antibiotics have no effect at all and should not be given.
The correct treatment depends on how much risk there is of a Pulmonary Embolism (PE) developing. This is assessed by a duplex ultrasound scan, performed by specialists who treat veins all of the time.
It is essential that if a diagnosis of Phlebitis of the legs is made, a duplex ultrasound scan is arranged as soon as possible to make sure that the correct treatment is started. In addition, the same duplex ultrasound scan will be able to diagnose the underlying cause of the Phlebitis, usually varicose veins or hidden varicose veins. Based around the results, a treatment plan can be put together to prevent the Phlebitis occurring again.
What Causes Phlebitis Of The Leg?
Phlebitis is the natural reaction for a vein that has been damaged and can occur in any vein in the body. Either the vein wall becomes inflamed, leading to a clot in the vein, or a clot forms in the vein itself, leading to inflammation of the vein wall.
Most phlebitis occurs in the legs and is caused by varicose veins or hidden varicose veins. There are other veins that get phlebitis and other causes, and so we will look at some of the more well-known ones here.
Varicose veins and hidden varicose veins
The commonest cause of phlebitis is the clotting of blood in varicose veins or hidden varicose veins.
Blood will clot when one or more of 3 factors are affected (collectively known as Virchow’s Triad). These are:
- Changes in the blood
- Changes in the blood vessels wall
- Changes in the blood flow
In varicose veins, the valves do not work and so blood flows backwards down the veins. This is a change in the blood flow. In addition, the flow is turbulent which stretches the vein wall to become varicose. This is the second change ie. change in the blood vessel wall. Either one of these changes by themselves could cause a clot and phlebitis. It is little wonder when both occur together that phlebitis occurs so frequently with varicose veins and hidden varicose veins.
Infusion or ‘drip’ phlebitis
Phlebitis can occur in any veins that have medication or fluid injected into them. This is often a reaction of the vein wall to the chemical that is being infused into the blood stream or the cannula (tube) that is inside the vein delivering an infusion. For example, it is very common to find hard, lumpy and tender veins in the arms of hospitalised patients who have had (or still have), a drip going into the vein in question.
These hard lumpy veins are usually blocked by the clot (thrombus) that accumulates inside the vein. With time, the clot usually resolves, opening the vein up again. However the vein wall may have become irreparably scarred and may either fibrose and disappear away as a scar, or may keep getting new bouts of phlebitis in it.
Malignancy or blood disorders
There are some rarer causes of phlebitis. Certain medical conditions such as some cancers or blood disorders (where the blood becomes thicker and more likely to clot) can cause different veins to suddenly clot unexpectedly around the body. This is a specialised area and we will not discuss it in more detail here. However, if a person suddenly starts getting phlebitis in more than one area for no apparent reason, they should see a doctor as soon as possible to try to find out why.
Malignancy or blood disorders
There are some rarer causes of phlebitis. Certain medical conditions such as some cancers or blood disorders (where the blood becomes thicker and more likely to clot) can cause different veins to suddenly clot unexpectedly around the body. This is a specialised area and we will not discuss it in more detail here. However, if a person suddenly starts getting phlebitis in more than one area for no apparent reason, they should see a doctor as soon as possible to try to find out why.
The Signs & Symptoms Of Phlebitis In The Lower Leg
As with every condition in medicine, phlebitis can appear in several ways. Although the following description is the classical presentational phlebitis, it is important to note that not everyone with phlebitis will have all of the symptoms and signs described here.
Most patients with phlebitis either get a sudden onset of the symptoms and signs, or a gradually increasing set of symptoms or signs over a day or two.
The first symptom is usually discomfort, tenderness or pain in one area of one leg (very occasionally two legs). This discomfort, tenderness pain is localised to one area usually running up the leg in the line of a vein. Depending on the vein affected, this might be vertically up the inner part of the thigh, diagonally across the upper thigh at the front, vertically up the inner aspect of the calf, vertically up the back of the calf or if there have been varicose veins before, phlebitis can be a series of lumps anywhere on the leg in the same position that the varicose veins had been.
Because the phlebitis is caused by a clot in the veins, the vein wall becomes inflamed and so the overlying skin also becomes inflamed. Therefore the skin overlying the area of phlebitis is usually red (unless it is very deep) and as the inflamed vein is under the skin, is usually tender to touch particularly if you push hard.
If the vein is superficial enough, a hard, lumpy, tender “tube” can be felt under the skin which is the clot and inflamed vein wall under the skin. If it is a set of varicose veins that have become thrombosed in the phlebitis process, then the lumps may feel more diffuse with one or more rounded mounds felt instead. However they will still be hard to the touch and tender on pushing.
Other conditions mis-diagnosed as Phlebitis
There are a host of other conditions that are mis-diagnosed as phlebitis. It is unfortunate that so many doctors and nurses use the term “phlebitis” whenever they see any inflammation or have a patient complain of a tender area in the lower leg. Not only is this usually an incorrect diagnosis but it often leads to the wrong treatment.
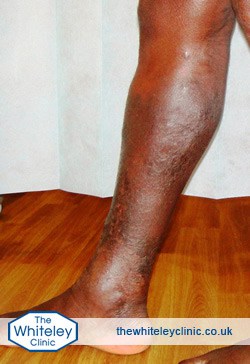
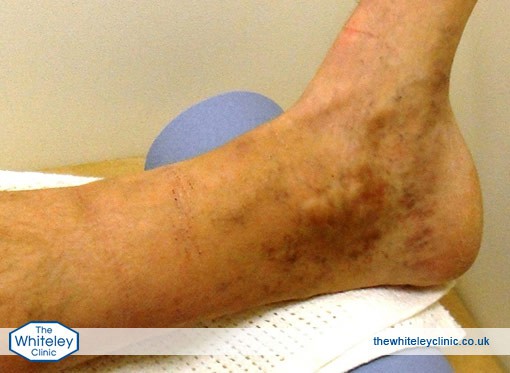
Severe haemosiderin and venous eczema of ankle and calf Venous eczema (or varicose eczema), lipodermatosclerosis, haemosiderin deposition, venous leg ulcer – all of these conditions are variations on the same problem, that of venous incompetence and venous reflux disease but without the clotting of blood in varicose veins or hidden varicose veins.
Severe haemosiderin and venous eczema of ankle and calf in black skin due to varicose veins -seen just below knee. This is not phlebitis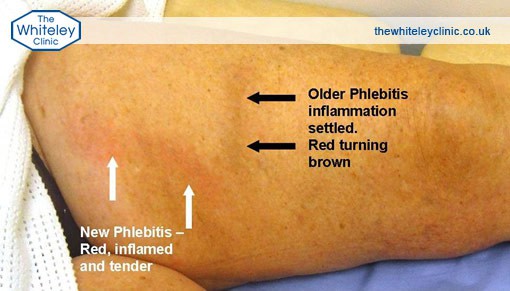
In these patients, the valves are not working in the leg and so when the leg relaxes, blood reflux is down the veins hitting the capillaries (very small blood vessels) in the skin at the ankles. Unlike phlebitis, where this process causes clots in the veins, in these cases the refluxing venous blood causes small amounts of trauma to the small vessels in the lower leg.
Although this does not have any immediate effect when it starts, after many years of repeated trauma, the tissue around the capillaries becomes inflamed and the skin starts to react. At first it gets irritated (venous eczema or varicose eczema), then it gets hardened and a little swollen (lipodermatosclerosis), then it goes brown (haemosiderin deposition) and finally it breaks down, causing a venous ulcer.
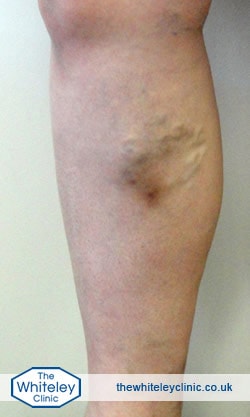
Atrophie blanche – skin of ankle is about to break down into a venous leg ulcer. The cause is venous incompetence causing venous reflux disease (or “hidden varicose veins”). This is NOT phlebitis.
In all of these conditions, the treatment is to stop the blood from refluxing down the veins – in other words to investigate and treat the venous incompetence stopping the venous reflux. This is completely different from the treatment of phlebitis.
Ultrasound Scans & Tests for Phlebitis
If phlebitis is suspected or diagnosed, it is essential to have a venous duplex ultrasound scan performed by a specialist who scans veins every working day.
Not only does the venous duplex ultrasound scan confirm the diagnosis of phlebitis, it also shows the extent of the phlebitis and allows for an accurate treatment plans to be identified.
Not having a venous duplex ultrasound scan can make diagnosis difficult and many people who are diagnosed clinically as having phlebitis actually have other conditions such as cellulitis, venous eczema or lipodermatoscleosis. The treatment for all of these other conditions is different and missing the need for anticoagulation medication such as Warfarin can be very dangerous.
Even if the venous duplex ultrasound scan confirms the diagnosis of phlebitis, the correct treatment depends on how extensive the phlebitis is, and whether it is extending towards, or even into, the deep vein.
Finally without a venous duplex ultrasound scan, the underlying cause of the phlebitis (usually varicose veins or hidden varicose veins) won’t be found and so the appropriate preventative treatment to stop it coming back again won’t be identified.
In most people, phlebitis is a relatively minor condition that needs a venous duplex ultrasound scan to confirm diagnosis and then aspirin and support stockings in the short term, with varicose vein surgery planned for the future to prevent recurrence.
However in some cases, the venous duplex ultrasound scan shows extension of the clot to within 5cm of the deep system, or even into the deep system, becoming a Deep Vein Thrombosis (DVT) which might potentially move to the lungs (known as a pulmonary embolism or PE).
This is a potentially serious, or even lethal condition which needs to be treated urgently with anticoagulation such as Warfarin.
Any delay in getting a specialised venous duplex ultrasound scan after a diagnosis of suspected Phlebitis can be detrimental to a patient’s health.
Specialist Phlebitis Treatment
In the past, doctors and nurses used to think that phlebitis (properly called superficial venous thrombophlebitis) of the leg was a simple condition that caused pain and discomfort, but never caused any risk to the patient. Unfortunately this has proven to be wrong.
Research and recommendations published between 2010 and 2012 have shown that the clots in the superficial veins that cause phlebitis can extend into the deep veins causing a deep vein thrombosis (DVT) and can also fly off to the venous system causing the potentially very serious pulmonary embolism (PE).
Therefore the old treatment of making the diagnosis clinically and without a scan, and then treating with aspirin (or even worse antibiotics), heat or cold compresses and support stockings is now a completely outdated and could potentially allow a serious or even potentially life-threatening condition to develop.
As such the American College of Chest Physicians and the British Committee for Standards in Haematology have produced guidelines that help doctors get the very best diagnosis and treatments for their patients.
The Whiteley Clinic have developed a protocol to investigate and treat patients with phlebitis or suspected phlebitis based on these guidelines.
Treatment of acute phlebitis
As soon as phlebitis (superficial venous thrombophlebitis) is suspected or diagnosed, an urgent venous duplex ultrasound scan should be arranged. This scan should be performed by specialists used to looking at veins.
The venous duplex ultrasound scan has two main functions in the diagnosis of phlebitis:
- Firstly to check if the phlebitis has an underlying deep vein thrombosis (DVT) associated with it
- Secondly to check the position and extent of the clot in the superficial veins that is causing the phlebitis
Using the results of the scan, the correct treatment can be selected.
If an underlying deep vein thrombosis (DVT) is identified, then it is the DVT that needs urgent treatment and anticoagulation (blood thinning medication) will be started immediately unless there is a very serious reason not to do so.
If there is no deep vein thrombosis (DVT) but there is extensive clot in the superficial veins that is at risk of causing a deep vein thrombosis, then it is recommended to start anticoagulation (blood thinning medication) to stop the clot extending and forming a deep vein thrombosis (DVT) and possible pulmonary embolism (PE).
If there is a reasonable amount of clot, but at less risk of causing a deep vein thrombosis (DVT) then it is recommended that a course of injections of heparin is started for several weeks. Once again this reduces the risk of clot extending.
If the scan shows that there is only a small amount of clot causing the phlebitis, then aspirin or other non-steroidal anti-inflammatory drugs can be used to reduce inflammation and pain.
Of course if the scan shows there is no clot underlying the phlebitis, then it will show the diagnosis was wrong and the correct treatment can be started for whatever the problem actually turns out to be – often a local infection called cellulitis.
In virtually all cases, graduated pressure stockings will also be used both to give the patient comfort and support as well as to further reduce the risk of extension of the clot in the veins and therefore reducing the risk of worsening phlebitis, deep vein thrombosis (DVT) and pulmonary embolism (PE).
Late treatment of phlebitis (prevention of further phlebitis)
We know that almost all phlebitis in the legs is due to varicose veins or hidden varicose veins. We also know that varicose veins and hidden varicose veins are caused by venous incompetence and venous reflux. Thus treatment of the venous incompetence will stop the venous reflux and therefore treat the varicose veins or hidden varicose veins. This will prevent any further phlebitis.
As with all varicose vein and hidden varicose vein treatments, these are now best performed by investigating which veins require treatment with a specialised venous duplex ultrasound performed by a specialist vein unit. This test will allow vein experts to select the appropriate endovenous treatment to get rid of the veins for good. This will usually be one of the thermoablation methods such as EVLA or “EVLT” (endovenous laser ablation or endovenous laser treatment), RFA (radiofrequency ablation), or one of the other methods such as TRLOP (transluminal occlusion of perforators), glue or mechanicochemical ablation (MOCA).
These thermoablation methods may need to be backed up with other more specialist treatments such as coil embolisation of pelvic veins, ultrasound guided foam sclerotherapy or phlebectomies – which are rarely sufficient treatments by themselves.
Treatment of the underlying varicose veins using the methods outlined in The Whiteley Protocol® will give both the lowest possible chance of getting phlebitis back again in the future as well is getting the lowest possible chance of developing recurrent varicose veins.
